26 April 2020
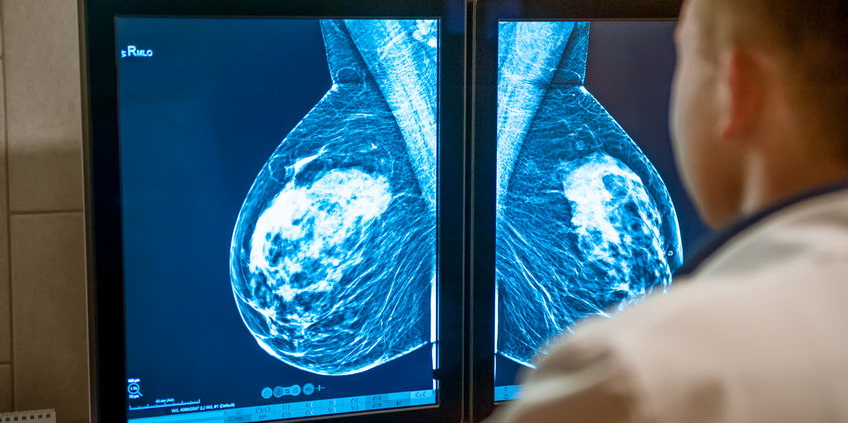
A study published in the Annals of Internal Medicine addresses the use of screening mammography in older women*. The goal of screening mammography (performed on a woman with no suspicious abnormality) is to reduce the likelihood of death from breast cancer. However, there are no randomized studies demonstrating this benefit in older women – they simply were not included in the early studies of screening mammography. Some national guidelines, including from the US Preventative Services Task Force, do not recommend screening mammography past age 75, noting that “the current evidence is insufficient to assess the balance of benefits and harms of screening mammography in women aged 75 years or older.” Some organizations, such as the American Society of Breast Surgeons and the American Cancer Society, recommend that screening mammograms continue as long as life expectancy is at least 10 years. In their Choosing Wisely statement, the American Geriatrics Society recommends that screening tests be considered in the context of life expectancy and take into account the risks of testing, overdiagnosis and overtreatment.
This study used data from Medicare to compare death rates in women age 70 – 84 who underwent screening mammography versus those who stopped screening. Patients had no personal history of breast cancer and had a life expectancy of at least 10 years.
There were slightly more breast cancers detected in the screening group, as expected: 5.5% in the women who underwent screening mammograms versus 3.9% in the women who did not. However, the researchers found that screening did not improve the likelihood of death from breast cancer. Among women age 70-74 there was 1 fewer breast cancer related death per 1000 women, over a period of 8 years, and this was not statistically significant. Among women age 75-84, there was no difference in breast cancer related deaths.
The authors concluded that screening mammography in older women does not significantly impact the likelihood of death from breast cancer. Limitations of this study include that it was an observational study, using information already in a database. The researchers could not adjust for certain factors including use of hormone replacement therapy, family history of breast cancer, and age at first pregnancy, which may impact breast cancer risk.
A separate study* looked at the use of a decision aid in patients age 75 and older. The decision aid provided information about the risks and benefits of screening mammography. In this study of 546 patients, it was shown that receipt of the decision aid prior to an appointment with their physician resulted in women being more knowledgeable about screening mammography and having more discussions with their doctor about screening. In addition, 9% fewer women opted to undergo a screening mammogram. The authors concluded that the use of a decision aid may help reduce over screening in older women.
In the accompanying invited commentary, Drs. Elmore and Ngo-Metzger noted that in women age 74 with average health and life expectancy, screening mammograms prevent approximately 1 death per 1000 exams. However, 1000 women being screened can result in 79 – 96 of them experiencing a false positive (“false alarm”). They pointed out the challenges of screening mammography in older women in that the reduction in death from breast cancer can take many years, (during which the woman may die from other causes) but the potential harms are more immediate.
These two studies and the editorial raise important questions regarding the routine recommendation for screening mammography in older women. The decision whether or not to continue screening should be based on breast cancer risk as well as general health and risk of severe illness or death from other causes. When to stop screening mammography is a challenging, but important conversation to have with our older patients.
- Additional Information:
- Annals of Internal Medicine article summary for patients
- New York Times Aging out of the Mammogram
- E-Prognosis mammogram decision aid, women age 75 – 84
- E-Prognosis mammogram decision aid, women age 85 and older
*If you are not able to access the full study and would like a copy, please email me: contact at drattai dot com